Fractional treatment of rosacea by LBO 532 nm laser with “one shot” procedure: A preliminary study
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Authors
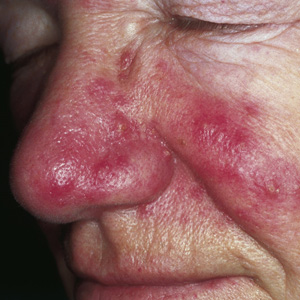
Rosacea is a chronic skin disease prevalently affecting the center of the face. The permanent erythema of skin face represents its typical sign. Further common features are face flushing, telangiectasias, and inflammatory presence of oedema, papules and pustules. The aim of this study was to investigate the use of LBO 532nm laser in the treatment of this disease. Ten subjects of both sex and middle age affected by rosacea in erithemato/teleangectatic stage were treated by a LBO 532nm laser single session. Discomfort evaluation during and after the treatment, one session results as well as incidence of the side effects were evaluated, with 6 months follow up. Positive results were obtained after only one session in total safety with minimal patients discomfort and without undesired effects during treatment. The study confirmed International literature data suggesting the use of laser and light devices as elective treatment of this disease. IPL, dye lasers and 532nm laser are the devices more used and the last seems to represent the gold standard for 1,2,3 phototypes. This clinical trial, with the limitations due to the small number of patients, indicated that “one session LBO 532nm laser treatment” represents an interesting and innovative approach in the therapy of the erythemato/telangectatic rosacea.
How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






